Understanding Fascial Fibrosis : the silent biological process that locks movement, drains energy, and fuels chronic pain.
This article is provided for educational and explanatory purposes only. It explores biomechanical and neuro-fascial mechanisms described in scientific literature and within the SBNFA™ systemic analysis framework. It does not constitute medical advice and does not replace diagnosis or care by a qualified healthcare professional.
Have you ever felt as if your body no longer truly “responds”? As if your lower back, pelvis, or shoulders have turned into a rigid shell that stretching, massage, or rest no longer seems to soften?
This sensation is often dismissed as fatigue, stress, or aging. In reality, it frequently reflects a precise and silent biological adaptation: fascial fibrosis.
In this article, we go beneath the surface of muscles and joints to understand how immobility, mechanical stress, and neural signaling can gradually transform supple connective tissue into a dense, restrictive structure — a process that profoundly alters movement, comfort, and energy.
📌 Key Takeaways — Fascia at a glance
- Fascia is richly innervated and plays a major sensory role in movement and pain perception.
- It represents a substantial portion of the body’s connective protein mass, primarily type I collagen.
- Prolonged immobility is associated with a marked reduction in postural micro-adjustments.
- A significant proportion of persistent pain syndromes involve fascial stiffening that remains undetected.
I. Fascia: From Silk to a Straightjacket
Fascia is a continuous connective tissue network that envelops muscles, nerves, organs, and vessels. When healthy, it behaves like wet silk: it glides, deforms, adapts, and redistributes forces smoothly.
Under prolonged mechanical stress, however, fascia can undergo a profound transformation.
During fascial fibrosis (#30), fibroblasts progressively differentiate into myofibroblasts. These cells no longer merely support structure — they actively generate tension. The tissue becomes denser, less deformable, and increasingly resistant to load, without conscious muscular control.
This is not a voluntary contraction. It is a form of biological sealing: the tissue adapts to perceived threat by stiffening itself from the inside.
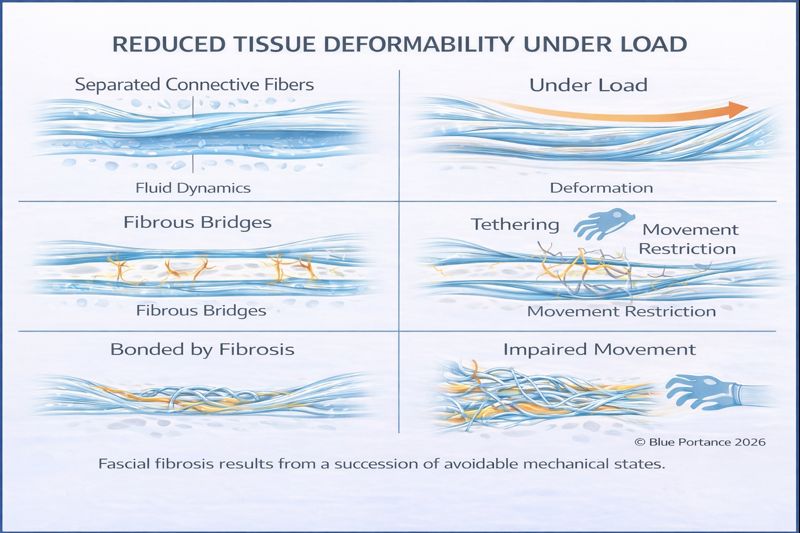
II. The Silent Culprit: Prolonged Sitting
Modern life requires prolonged sitting — often exceeding eight or nine hours per day. For fascia, this represents a major mechanical challenge.
A well-documented phenomenon known as creep (#15) explains why. When tissue is subjected to constant load without movement, water is gradually expelled from its matrix.
As hydration decreases (dehydration #28), collagen fibers come into closer contact. Without regular shear and glide, these fibers may form bridges and adhesions. Over time, the tissue “memorizes” the seated shape.
You stand up — but part of your body remains mechanically seated.
III. When Nerves Trigger Tissue Defense
Fascia does not stiffen in isolation. The nervous system plays a central regulatory role.
When a nerve becomes mechanically irritated (#36), it releases neurochemical signals associated with inflammation and tissue remodeling. This phenomenon — often referred to as neurogenic inflammation — alters the surrounding connective environment.
Rather than being passively compressed, the nerve can actively contribute to local stiffening, encouraging the formation of a protective but restrictive fibrous envelope.
This defensive response may reduce immediate mechanical threat, but it also increases sensitivity, reduces glide, and amplifies pain signaling over time.
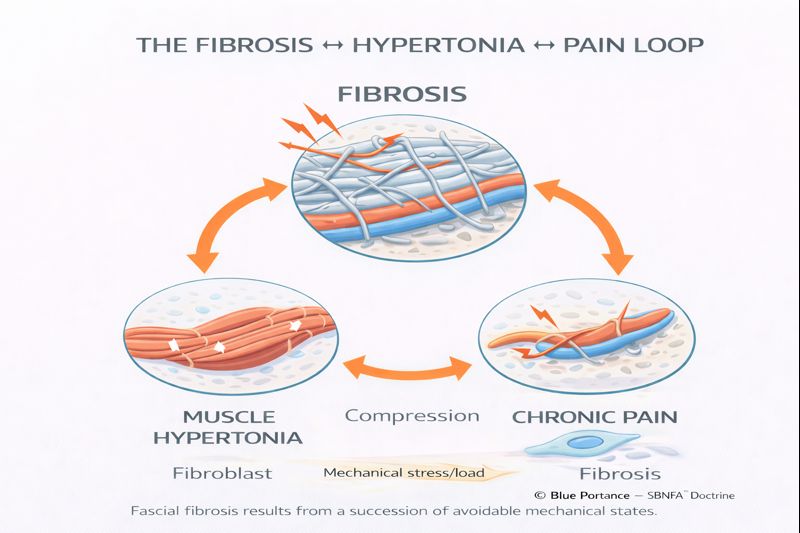
IV. Hypertonia: A Reflex, Not a Flaw
As fascial stiffness and neural irritation increase, the body activates a powerful protective reflex: persistent elevation of muscle tone, known as hypertonia.
Unlike voluntary contraction, hypertonia is unconscious and continuous. Muscles remain partially engaged even at rest, attempting to stabilize a system perceived as unstable.
- Muscles feel tense without obvious effort.
- Compression on nerves and tissues increases.
- Movement becomes restricted to avoid painful spikes.
Key point: hypertonia is not a defect. It is a protective strategy in response to altered mechanical information. As long as the underlying signals remain threatening, the nervous system maintains this state.
V. Micro-Movement: The Missing Signal
Contrary to common belief, recovery does not primarily depend on intense exercise. The decisive factor is often micro-movement (#14).
Subtle postural adjustments, breathing-related motion, and low-amplitude shifts provide continuous mechanical information to tissues. These signals regulate collagen turnover and enzymatic remodeling.
When micro-movement disappears, tissue maintenance mechanisms slow down. Collagen accumulates faster than it is recycled. Stiffness increases.
Research suggests that individuals with persistent pain exhibit a substantial reduction in these micro-adjustments, leaving tissues mechanically “silent.”
VI. The Cone of Economy: Why Fatigue Appears First
The body constantly seeks balance with minimal energy expenditure. This principle was elegantly described by Jean Dubousset as the Cone of Economy (#63).
Fibrosis acts like a shortened rigging line on a sailboat. It pulls the structure off-center. To remain upright, muscles must work continuously.
The result is hidden energy consumption. Even without visible effort, the body is fighting gravity all day. Adaptive reserve declines. Fatigue precedes pain.
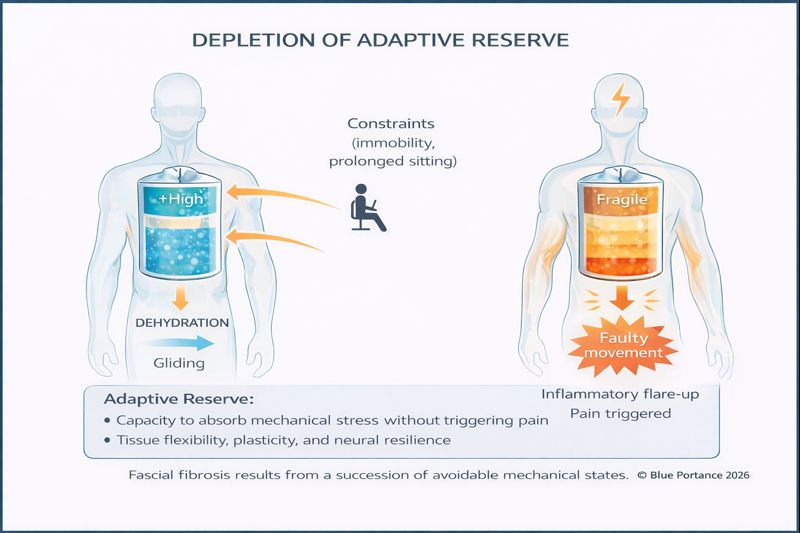
VII. Loss of Adaptive Reserve (#71)
In a healthy system, fascia absorbs unexpected stress. In a fibrotic system, this margin disappears.
Like aged plastic, stiffened tissue no longer stretches — it transmits force directly. Minor stressors become crises.
This marks the loss of adaptive reserve.
Conclusion: Restoring Mechanical Dialogue
Fascial fibrosis is not a sudden event. It is a gradual adaptation to immobility, repeated stress, and loss of tissue dialogue.
The solution does not lie in force or correction, but in restoring a soothing mechanical conversation: reintroducing glide, variability, and safe movement where rigidity has settled.
Key principles to remember:
Avoid prolonged static positions. Change posture regularly and allow micro-adjustments.
Use diaphragmatic breathing. It provides deep internal micro-movement and calms neural tone.
Listen to early stiffness. Morning rigidity often signals reduced glide.
Restoring even a fraction of daily micro-movement can reactivate biological remodeling processes. The body is an extraordinary adaptation system — when given the right mechanical signal.
👉 To explore this further, continue with: Why moving a little is more important than moving a lot .
References
- Adams & Dolan — Tissue creep and load adaptation.
- Stecco — Fascial glide and densification.
- Sundblad — Postural micro-adjustments and pain.
- Dubousset — Balance and energy economy.
© Blue Portance — Educational reproduction permitted with citation of the SBNFA™ framework.


